Navigating pregnancy-safe skincare can be complicated, but as a medical doctor with a focus on cosmetic ingredient safety, I’ve simplified the search for you. Visit my Skincare During Pregnancy – Begin Here guide for a full index of ingredient safety reviews, pregnancy and IVF-safe recommendations, and doctor-vetted product guides.
Today is about melasma, also known as ‘mask of pregnancy’, and chloasma, which is a common pigmentary disorder affecting women (90%) more than men (10%).
Presenting as brown to grey-brown flat patches anywhere on the face (forehead, cheeks, nose, chin, etc.), these, although entirely harmless, can cause significant stress, social anxiety, and self-consciousness.
Quick Navigation
- What causes melasma?
- Genetics.
- Influence of pregnancy hormones.
- Sunlight exposure.
- Medications & scented products.
- Heat Exposure.
- How to prevent melasma?
- What type of sunscreen is best for melasma?
- What is the right way to apply sunscreen?
- Can I use any preventive topicals while pregnant?
- Do I have a higher chance of developing melasma when pregnant?
- Can it turn cancerous?
- Takeaway.
What causes melasma?
The pigmentation that occurs in melasma is due to the overproduction of melanin ( a natural pigment found in our skin that gives it its color) by melanocytes (cells in the skin that produce melanin).
The female hormones estrogen & progesterone are said to stimulate the melanocytes to produce more melanin.
Thus, people with greater melanin in their skin (e.g., Latinos and Asians) have a higher chance of developing melasma during pregnancy.
The mechanism is similar to the development of age spots and freckles, but melasma spots tend to be much larger and more diffuse.
- Genetics
About 50% will report a positive history of melasma in a parent.
Individuals with skin of color and those who tan quickly have a higher prevalence rate due to a higher melanin content.
- Influence of pregnancy hormones
Up to 50% of pregnant women can develop melasma, making it so common in pregnancy that it is also known as the ‘mask of pregnancy.’
With pregnancy, there is an increase in the hormones estrogen and progesterone. These two, the latter in particular, stimulate the melanocytes in the skin, which produce the color-giving pigment called melanin.
It most commonly begins in the second and third trimesters of pregnancy.
In some cases, the melasma goes away once the pregnancy ends.
The role of hormones is important, as shown by the increased incidence of melasma in women on birth control pills or those taking hormone replacement therapy during menopause.
- Sunlight exposure
The sun is a big culprit and a potent trigger of melasma. Sunrays promote the production of melanin and cause hyperpigmentation.
Melasma often improves in winter and worsens as summer peaks.
The incidence of melasma is also higher in tropical regions.
- Visible light from your phone & laptop.
The light from your laptop and phone screens contributes to hyperpigmentation by activating melanocytes, which produce the pigment melanin, as shown by this oft-quoted study – Impact of long wavelength UVA & visible light on melanocompetent skin.
This effect is more pronounced in darker-skinned individuals as compared to lighter skin tones.
Like the effect of sunlight, the damage is cumulative and occurs over time.
- Medications & scented products
Certain medications for epilepsy, malaria, anti-psychotics, and cancer have been reported to cause hyperpigmentation.
Added scents in your skin care products are a source of allergen – this may not always be obvious in the form of redness or itching, but they can cause inflammation of the skin, which can kick-start the pigmentation process.
Added fragrance to your skin care products is just for the sensory appeal and contributes nothing to the actual benefits of the product you use.
These can be harmful for your health, as, unless specified, added fragrance is a concoction of dangerous chemicals known as phthalates.
Personally, I advise my patients to steer clear of added fragrance in skin and body care products.
- Heat Exposure
It has been suggested that exposure to an intense and prolonged source of heat, e.g., cooking fires for chefs, ovens for bakers, may trigger melasma, and the continued exposure may make it difficult to treat.
How to prevent melasma?
- General measures:
- Prioritise strict year-long protection from sunlight & visible light.
- No tanning beds or sunbathing.
- Reduce direct heat exposure, such as with ovens or cooking fires.
- Follow these basic skin practices:
- Use non-perfumed products.
- If you have sensitive skin, use cosmetics minimally, or if you must, use products tailored for sensitive skin.
- Avoid vigorous rubbing of products on your skin.
- Strict sun protection
Sun exposure is a potent trigger for melasma and also worsens it.
Furthermore, any precaution or treatment you undertake for melasma is negated if sun exposure continues.
Using sun protection every day and in the proper manner is a measure that cannot be underscored enough in the prevention and treatment of melasma.
- The measures for sun protection should be followed the whole year, even in winter or on cloudy days, as the UV light still filters through.
- Wear a broad-brimmed hat on sunny days when outdoors.
- Look out for shady areas when outdoors.
- Ditch tanning beds and sunbathing.
What type of sunscreen is best for melasma?
A tinted sunscreen of minimum SPF 30 with broad-spectrum protection is what you need for melasma.
Tinted because these have been shown to block visible light that emanates from your screens and LED lights.
Here are some guidelines:
- Minimum SPF of 30.
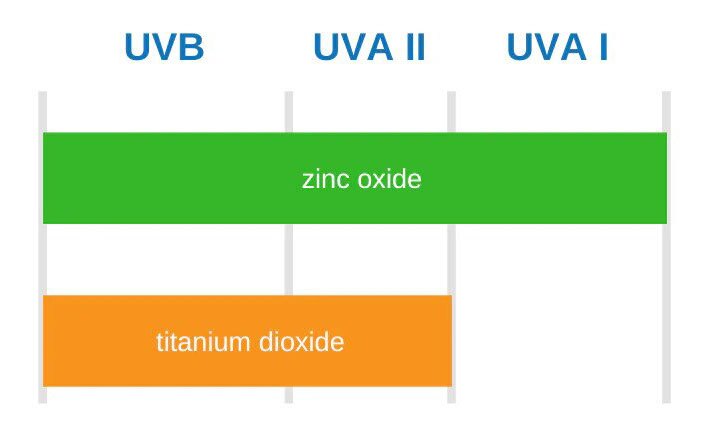
- Use a mineral sunscreen that is made primarily or exclusively of zinc oxide, as it has a broader spectrum of protection than titanium dioxide. Do not buy it just because it says ‘mineral sunscreen’ on the bottle.
Many times, the mineral component may not be the one you need or might be just loaded with chemical sunscreen, with just a fraction of mineral ingredients.
Source: Waxhead Sun Defense - Always use tinted sunscreen. The iron oxides used in tinted sunscreens have been shown to protect against visible light.
Furthermore, tinted sunscreen will save you from the white cast that comes along with mineral sunscreen.
*Iron oxides in topical products are safe to use in pregnancy. - Use a cream or lotion formulation. Avoid spray-ons or powders that result in uneven and inadequate protection. You may use a powder on top of your suncream or lotion for aesthetic purposes, but do not depend on it for any protection.
- Mineral sunscreens can be unpleasant to use as they have a heavier texture and leave a white cast. Using a tinted version and nanoformulation will help with the white cast.
- Mineral sunscreen is not only the type of sunscreen that is recommended to be used for melasma, but also the only type that is considered safe to use in pregnancy. Chemicals sunscreen should be avoided during pregnancy.
- Most importantly, read the FULL ingredient list. You do not want to be so focused on using a product containing mineral sunscreen that you bypass the ingredients that are potentially harmful to use when pregnant.
- I have blogged about these ingredients in the following posts:
– Part I: IVF & Pregnancy Safe Skincare- Avoid These Ingredients.
– Part II: IVF & Pregnancy Safe Skincare- Avoid These Ingredients.
– Safe Skincare for Nursing Moms- Ingredients to Avoid.
– Parabens In Cosmetics: Are They Safe To Use?
What is the right way to apply sunscreen?
As the AAD (American Academy of Dermatology) has rightly said, ‘Sunscreen only works when applied correctly.’
No matter how high an SPF or how renowned or expensive a product you may choose, unless applied correctly, you not only gain no benefit from it, but you may end up harming yourself (sunburn, for one) by being in a false illusion of being protected.

For the head, face, & neck area, squeeze out 2 thin strips of sunscreen on the whole length of your index and middle finger- that is how much you must be using- The Rule Of Nines.
For only the face and neck area, 1 finger should suffice.
Or

For just the face and front of your neck, for most people, ¼ teaspoon will suffice.
Consider using more if you have a high forehead, and for application to the back of the neck.
To simplify things, aim between ½ and ¼ teaspoon for the face and neck.
And remember that sunscreen should be reapplied every two hours or more frequently if swimming, sweating, or toweling off.
Can I use any preventive topicals while pregnant?
During pregnancy, chloasma does not require any particular treatment besides the use of an effective sunscreen, sun protection with caps, etc., and avoiding the use of any photosensitizing products or an inappropriate skincare routine.
There is a good body of evidence in the medical literature about the efficacy of sunscreens.
- A study conducted on 200 Moroccan women who were <3 months pregnant showed that the use of a broad-spectrum high SPF of 50 resulted in only 2.7% developing melasma compared to 53% in the same time period and geographical area as studied by the same investigators.
The study also found improvement in 8 of 12 women who had pre-existing melasma. - This study evaluated the role of sunscreen alone in melasma and concluded that there was a statistically significant improvement in melasma after 12 weeks of sunscreen alone, which also improved the quality of life of the patients.
Do I have a higher chance of developing melasma when pregnant?
As mentioned above, the following factors increase the risk of melasma:
- Individuals with skin of color
- History of melasma in a parent.
- Repeated and frequent exposure to triggers like sunlight, visible light, or sources of high heat
Another risk factor that has been identified is that if you have a history of melasma or hyperpigmentation when on hormonal contraceptives (oral pills, implants, IUDs, vaginal rings, skin patches), you have a higher risk of melasma when pregnant.
In this study, 87% of the test subjects having melasma from oral contraceptives also developed it during pregnancy.
Can it turn cancerous?
No, melasma is not a form of cancer.
It is also not a precancerous condition or a sign of skin cancer.
Takeaway
- Melasma in pregnancy happens due to hormonal changes, which stimulate the melanocytes to produce more pigment.
- People of color, positive family history, those on certain medications, history of pigmentation changes with hormonal contraceptives are more prone to develop melasma during pregnancy.
- Not just sun exposure, but visible light from your phone and laptop is involved in the pathogenesis.
- Sun protection with physical barriers (umbrella, hats) and use of a minimum SPF 30 broad-spectrum sunscreen with iron oxides (i.e.tinted) for visible light should be prioritised and is the number one step in the prevention and treatment of melasma.